People with autoimmune diseases or any chronic illness are at an increased risk for having mental health issues, especially anxiety and depression. While dealing with a mental health issue alone has an extreme effect on a person’s health, having a mental health issue in conjunction with a chronic illness could potentially be worse. It has been found that up to 50% of patients with autoimmune diseases have shown an impairment in their health-related quality of life which can then lead to the person exhibiting depressive symptoms.
The mind and body have a connection that goes both ways. Because of this, conditions, such as chronic illnesses and autoimmune diseases can have an impact on how you think and feel and therefore your thoughts and feelings can impact autoimmune diseases symptoms. It doesn’t end there though, a newer study in the Journal of the American Medical Association has found that stress may actually cause autoimmune diseases. This study found that individuals diagnosed with a stress-related disorder were more likely to be diagnosed with an autoimmune disease and were more likely to develop multiple autoimmune diseases. Stress causing physical symptoms isn’t a new concept though. Numerous studies have found that stress wreaks havoc on our bodies. And it just isn’t extreme stress from a traumatic event, it can be life’s daily stressors.
What exactly is stress? It is any experience that can cause tension, whether it is physical, psychological, or emotional. This is even worse if the stress sets off the fight or flight response. The fight or flight responses is our bodies response to stress in which the adrenal gland releases adrenaline which then leads to a rapid pulse and rapid breathing along with increased blood pressure. This response is fine when we are in an acute stressful situation, but this is very unhealthy when it is chronic or persistent stress (finances, health, relationships, anything that is considered a daily struggle). Think of your daily stressors, how many times a day do you experience some type of stress that makes your heart rate increase a little bit along with maybe the butterflies in your stomach. Unfortunately, your body is physically going into the fight or flight response.

Those with autoimmune diseases will not necessarily have symptoms severe enough to be diagnosed with a mental health condition and those with a mental health condition or stress will not have symptoms severe enough to be diagnosed with an autoimmune disease, but that does not mean that you cannot still experience both the physical and mental symptoms on both sides. However, people with autoimmune diseases have reported having poor sleep, depressed moods, and a lower quality of life; therefore, it is always important to look for mental health symptoms.
How do autoimmune conditions cause mental health problems? Researchers and doctors do not fully understand how autoimmune diseases can cause mental health conditions, just like they do fully understand what causes an autoimmune disease to begin with, but they are aware of a mind-gut connection, a mind-immune connection, and a gut-immune connection. Other theories include inflammation. As I have discussed in previous blogs and podcasts, inflammation is a primary cause of autoimmune disorders, while also creating a plethora of symptoms. When we have an autoimmune disease our immune system is continuously fighting and therefore causes a major increase in the inflammation in different areas of our body and the inflammatory response continues which then can lead to significant tissue and organ damage.
This inflammatory response makes it extremely difficult to control the autoimmune process and to reduce the symptoms. In theory (and in some research studies), it has been found that if we can reduce the inflammation in the body, we will have remarkably reduced symptoms which would then control the autoimmune process. People with autoimmune diseases have higher levels are known as pro-inflammatory cytokines in their blood. These chemicals cause inflammation in the body while also affecting brain chemicals that regulate mood and energy levels. This process causes symptoms that are similar to depression, including fatigue and issues with sleep and appetite.
A second theory includes stress. The stress of dealing with an autoimmune condition may lead to mental health problems. Stress can produce changes in every system in our bodies and minds which then stimulates both physical and psychological reactions. The two major physical reactions are the fight or flight response and the general adaptation syndrome.
The fight or flight response happens whenever we perceive something stressful. In this response:
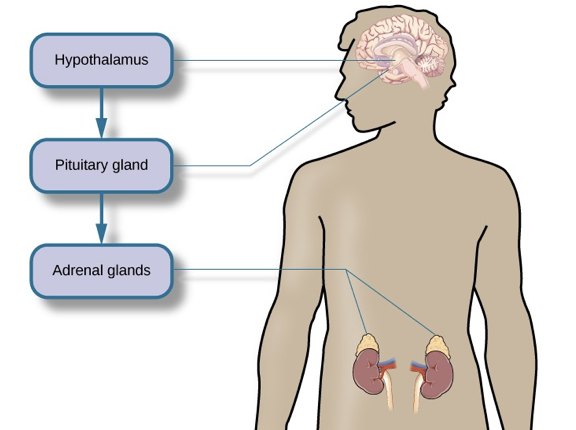
- The sympathetic nervous system releases adrenaline from the adrenal glands to activate the fight or flight response;
- At the same time, the hypothalamus releases corticotrophin-releasing factor, a hormone that causes the pituitary gland to release adrenocorticotropic hormone (ACTH);
- When the ACTH activates, the adrenal glands secrete cortisol, which helps provide that boost of energy preparing us to run away or fight.
This is why we tend to feel scared and anxious along with all the physical symptoms that come with those feelings. Think the increased heartrate, possibly trouble breathing or hyperventilating, a stomach ache, sweating, and flushed skin.
The general adaptation syndrome is a three-stage physiological stress response that appears regardless of the stressor that is encountered. It is very non-specific and does not vary across stressors. The three stages of general adaption syndrome are:
- The alarm phase which is the rapid mobilization of bodily resources that respond to the threat;
- The resistance phase which is the adaptation to arousal state and coping with a stress and;
- The exhaustion phase which is where the body’s resistance collapses, leading to infection, tumor growth, aging, irreversible organ damage, or death.
In the general adaptation syndrome, resistance to stress builds over time, but then can last only so long before exhaustion sets in. The constant exposure to stress leads to wear and tear on the body and accelerated aging. Additionally, chronic stress affects the immune response – stressors can cause hormones (glucocorticoids) to flood the brain, wearing down the immune system and making it less able to fight invaders. This creates a constant circle of stress and inflammation in the body and the effects of chronic stress wreak havoc on our body as the increases in cortisol can significantly weaken our immune system and are associated with depression. This stress also contributes to the development of psychological disorders.

The third theory is the psychological effects of having an illness. When a person is diagnosed with an illness (any type of illness), it leads to a sickness response which is a coordinated, adaptive set of reactions to illness organized by the brain and can be prompted through stress without having an active infection. With the sickness response, the immune system begins with the activation of white cells and cytokines which are released and activates the vagus nerve and induces an I am sick message. Because a person with an autoimmune disease already has an overactive immune system, this too creates a constant vicious circle. Furthermore, stress hormones inhibit the production of lymphocytes which are white blood cells that are important in the immune response. This leads to people with higher stress levels or chronic stress to be more likely to get sick when exposed to a cold, show poorer antibody responses following vaccinations and slows down wound healing. The connection between this sickness response and the immune response is usually illustrated with depressive symptoms. Additionally, it can lead to what is called somatic symptoms disorder which is a hypersensitivity to symptoms or to the possibility of illness that underlies a variety of psychological problems and can then create a psychosomatic illness as well.
It doesn’t stop there though, a study in Denmark found that depression and other mood disorders could be the brain’s response to inflammation. This just shows how much inflammation plays a part in our body and how important it is to control that inflammation. Inflammation is the body’s protective response to an infection, while autoimmune disorders are inflammatory conditions caused by the body’s overreaction to naturally occurring substances and tissues. Researchers have found that patients with an autoimmune disease were 45% more likely to have a mood disorder, while any history of infection increased the risk of a mood disorder by 62% and about one-third of people diagnosed with a mood disorder had been hospitalized in the past for a serious infection or illness.

Leave a comment